|
With good planning, however, it’s doable and very worthwhile. Not only will your baby still receive the best possible nutrition via your milk, but it will be an easy and lovely way to reconnect with your baby at the end of your working day.
Even if you aren’t able to pump enough to meet all your baby’s milk needs for when you’re not together, partial breastmilk-feeding is still very valuable; it doesn’t have to be “all or nothing”. Every drop you provide for your baby is priceless – which is why some people call it “liquid gold”. There is such a huge amount of information available on the internet nowadays that it can sometimes be hard to know where to start, so we’ve put together this summary of all the information you’ll need to help the process go as smoothly as possible. You’ll notice there are some sentences highlighted in blue: these denote things which can help boost your milk supply which we will cover in more detail later. Childcare and flexible work options Most people start by looking at which pump to buy, but we think it’s important to first consider your work routine and your childcare options, to see if there is scope for reducing the length of time that you need to be separated from your baby. Some organisations allow employees to work from home or take some work home with them some days – at least for a short period. Investigate whether there are childcare options near your workplace, which would reduce your hours of separation and may allow you to visit your baby during your lunch hour. If your spouse or another close family member will be looking after your baby, they may be willing to bring your baby to you for a feed. Even if you think those suggestions are out of the question for you, it’s still a good idea to have a chat to your HR department or boss in advance of starting work to discuss the arrangements. If you have a Monday-to-Friday job, discuss the possibility of returning to work on a Thursday or Friday. Taking the next two Wednesdays off (or asking to work those days from home) also helps: you would then work no more than two days in a row for the first 2.5 weeks, allowing you and your baby a much gentler transition. You’ll need to discuss where and when you will be able to pump. Ask colleagues who have pumped in your workplace what they recommend. Explain that you will probably need a 20-minute break at least every three hours. Emphasise that your needs are only temporary, and that there are good business reasons for companies to support breastfeeding mothers. Consider sharing this guide to establishing a breastfeeding-friendly workplace, or find one relevant to your country. When to introduce bottles to your baby To get breastfeeding off to a good start, it is recommended to wait until breastfeeding is well established (usually around four to six weeks) before introducing a bottle. Introducing bottles too early can make it harder for babies to learn how to breastfeed effectively. If your baby needs any supplementary milk during those early weeks, it’s preferable to use a special baby feeding cup, syringe or spoon. Bottles are the most practical option to feed babies expressed milk on a long-term basis, but it’s important that your caregiver feeds in a breastfeeding-friendly way. They should use the slowest teat that your baby will tolerate, ideally a newborn one (so your baby is less likely to get frustrated with the ebbs and flows of milk at the breast) and use “paced bottle feeding”, explained by this video and this print-out. Once breastfeeding is going smoothly, you’ll want your baby to have some practice with bottle-feeding in advance of your separation period. But it’s best to continue to focus on direct latching, because too much bottle-feeding can result in “nipple confusion”, have a negative impact on your milk supply, and deplete your freezer stash. If your baby doesn’t take to the bottle easily, we recommend backing off and trying again another day. You can also try some of these great tips to introduce a bottle to a breastfed baby. At the age of six months, most babies are able to start learning to drink from a “sippy cup” or a straw, at which point you may be able to avoid bottles altogether. Which pump? If your baby is less than six months old and you will be going out to work full-time, you should invest in the best pump you can afford. The highest grade pump is known as hospital-grade. Until recently, these were only available for rent, but some brands are now manufacturing hospital-grade pumps at retail prices. The next grade down (and more portable) is a fully automatic double-electric pump which will cost a few hundred US dollars. You can also explore the option of renting a hospital-grade pump – ask your local LLL Leader, IBCLC or hospital about local rental options. Note that if you’re considering buying a second-hand pump, you need to know whether it has a closed system or an open system. It’s not recommended to share parts which have been in contact with somebody else’s milk, because sterilisation doesn’t kill all communicable diseases. With a second-hand closed system pump, you can buy an extra set of the milk-contact parts, which will be cheaper than buying the whole pump new. The most economical pumps will cost less than US$100 and are suitable for occasional or once-daily use. They are not recommended for maintaining your milk supply while separated from your baby several hours a day. Although not many working mums rely solely on hand-expression of milk, some report that they can express more through hand-expression than through mechanical means – check out this video showing a good method, which is worth everyone learning in case of an emergency. Hand-expression can also be useful for those times when you only have five minutes to spare and it’s not worth your pump’s set-up and pack-away time. Choose the most suitable pump for your work situation. If you always work in the same place and will have regular breaks in a designated pumping room, a hospital-grade pump may be a good option. These can sometimes be heavy and noisy, so you may also need to buy a cheaper pump to keep at home as well. If you are often on the move, you will definitely need a more portable and quieter option. If you expect it will be difficult to carve out break times away from your desk, you may choose a brand that allows discreet pumping from inside your bra. It’s important to make sure pumping is comfortable to prevent nipple damage and maximise output. Start with a low suction setting and only increase the suction once it’s comfortable.
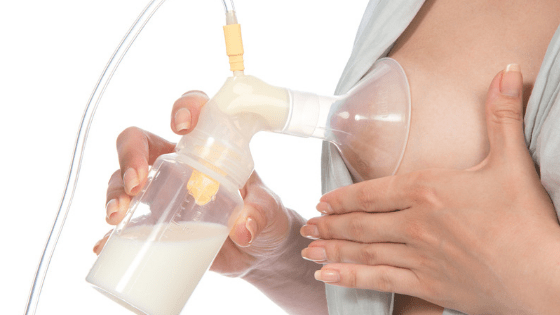
Pumping – when and how to get started
We recommend waiting until about a month before your separation begins, for several reasons:
Regardless of the stage at which you decide to begin pumping, it cannot be stressed enough that the amount of milk you are able to pump is NOT a reliable indicator of how much milk you are producing or how much milk your baby is drinking. A baby who is breastfeeding well is much more efficient than any pump. Pumping also takes practice – your breasts will respond better the more often you pump – and it's totally normal to only pump 30-60ml if you pump after nursing at the breast. A good strategy to get started is to pump a small quantity two or three times a day, and combine the chilled milk from all sessions that day to store in the freezer. It’s best to freeze in 60-90ml/2-3oz batches at first, to reduce the risk of wastage. Once your separation period has started
If your schedule allows, plan to breastfeed at least twice in the morning before leaving your baby. If you are dropping your baby off at daycare, breastfeed upon drop-off and/or pick-up. Suggest to the caregiver that if your baby seems hungry shortly before you arrive, they should only feed a small amount which won’t spoil your baby’s appetite for breastfeeding.
An added advantage of nursing your baby at daycare is that your milk has a chance to respond and adapt to any germs in that environment. Breastmilk is quite incredible! What to take with you to work. Here is a non-exhaustive list (some items can be left at work):
When to pump: First thing in the morning, after baby's first breastfeed, is usually a good time because your breasts may still be relatively full (assuming your baby’s longest stretch of sleep is at night). Others find they have more time for pumping after baby first goes to sleep for the night. Pumping once during the night, sometime between 1am and 5am, can also give a good yield due to higher levels of prolactin (the hormones that tell your body to make milk) – skip this if you are already breastfeeding a few times during the night. To fit pumping into your working day, try blocking your diary if possible and setting reminders. Lunch breaks can be a good time to get a consistent pumping session in. Consider pumping at your desk so you can continue getting work done, with a cover-up if necessary. If you have a pump that fits inside your bra, you can even pump while on the move or during meetings. Alternatively, use a “pumping bra” – you can either buy a ready-made one or make your own by cutting up an old or cheap bra – there are several different methods to be found on YouTube. Consider pumping before starting your work day and right after work, even if only for 5 minutes. How often to pump: This varies from person to person, as everyone has a “magic number“ of times per day that their breasts need to be drained to maintain their milk supply. If your baby currently breastfeeds eight times per 24 hours, you will need to continue draining your breasts at least eight times each day. How long to pump for: This really depends on how much time you have and how long it takes for your breasts to be well drained. If you have time, waiting for a second letdown can make a big difference. It may take 10 minutes from the first letdown until it slows down to a trickle; you can then switch back to massage mode to stimulate a second letdown, and then switch to expression mode for another 5 to 10 minutes to really fully empty the breast. How to maximise pumping yield: It’s important to be as relaxed as possible when you pump, which encourages letdown. Make your surroundings as comfortable as possible (toilets are NOT conducive for this!) with extra cushions if desired. Consider audio-visual options: relaxing music, meditation tracks, or even a recording of your baby crying! Some people find that focusing on their baby (photos or videos can help) encourages letdown; others find that they feel more relaxed if they are distracted by something (such as a book or video) which has nothing to do with their baby. Try closing your eyes and visualising waterfalls; experiment to find out what works for you. It can also help if your breasts are warm: go for a brisk walk or climb some stairs before pumping, apply something warm to your breasts, and/or drink something warm. Definitely DON’T focus on how much you are pumping (unless you find it easy to pump a lot) because anxiety inhibits milk flow. Be proud of every drop of “liquid gold” that you are pumping. Learn about how this hands-on pumping method can help to fully empty your breasts. If you find that the amount you are able to pump is not keeping up with what your baby is drinking, the first thing to do is to check whether your baby might be drinking too much when bottle-feeding. Caregivers need to be informed that a breastfed baby needs slightly less milk than a formula-fed baby, for two reasons. Firstly, breastfed babies may drink more milk when their mothers are around, and this is fine so long as they are getting what they need over every 24-hour period. Secondly, breastmilk is more easily digested and so fewer calories are required for the digestive process. Check out this "milk needs" calculator for the exclusively breastfed baby that’s good to share with your baby’s caregiver. It’s also good to remember that babies have a temporary increase in milk needs during growth spurts and developmental milestones, in which case things should calm down within a few days. If you really do need to pump more, here are some great tips to boost your supply. In addition, you can look into “power pumping”, which follows the principle that frequent, short pumping sessions are more effective than infrequent, longer sessions if the overall time spent is the same. There are two methods, one involving frequent short pumps during a one-hour period, for at least a few days in a row, and another involving leaving the pump handy for a few hours. You can also refer back to many points highlighted in blue earlier which could help your milk supply, and speak with a LLL Leader or IBCLC who will analyse your situation and give individual recommendations. If nothing helps and your baby needs supplemental milk, the first choice is donor milk if you can find a reliable local source. If your baby is over six months old, you also have the option of giving more solid foods while you are separated and letting your baby catch up on milk intake when you are together. If you can’t quite pump enough, it’s also worth remembering that partial breastfeeding is always better than no breastfeeding. Pump cleaning and milk storage Milk storage and handling guidelines are clearly set out in this LLL article. Here is a quick reference guide from KellyMom that is good to stick on your fridge and/or give to a caregiver. Some people recommend keeping pump parts in the fridge between uses and only washing thoroughly and/or sterilising when they get home at the end of the day. This can be a big time saver and is worth considering, although it is against the latest CDC guidelines. Washing your pump thoroughly after each use is always advisable if your baby is under three months (adjusted age if premature) or is unwell. The case for keeping your pump parts in the fridge is increased if there is nowhere hygienic in your workplace for the washed or sterilised parts to air-dry, or if you don’t have time to wash thoroughly with soap and water – just rinsing with water can cause bacterial growth. Sterilisation is not mandatory for human milk containers and pump parts (unlike items which have been in contact with cow’s milk or formula) because human milk has antibacterial properties, but it’s still recommended for babies under three months, sick babies, if you don’t have access to hot water, or if you don’t trust another caregiver to wash the parts carefully. You may have heard that human milk is tailored to each baby’s age. This is true, but milk that you pumped two months old ago is still much better for your baby than formula. While some people like to follow a strict “first in, first out” policy for expressed milk (putting everything in the freezer to ensure that the oldest milk gets used first), some find it more convenient to primarily use refrigerated milk, because it’s easier for caregivers to warm up chilled milk than to defrost frozen milk. We hope this overview will help empower you to continue breastfeeding if you are separated from your baby. Remember to reach out to your local LLL leader if you encounter problems or just need some encouragement to keep on pumping. We are here to help! Close to the Heart Vol. 20, No. 1 (Early-Year 2019) Please contact the editor for Close to the Heart at [email protected] if you have a breastfeeding story you would like to share.
Comments are closed.
|
Close to the Heart ArticlesCategories
All
Close to the Heart is protected by copyright law. Reproduction and/or use in any form, by any means, graphically, electronically, or mechanically, is prohibited without permission.
|
Our Mission is to help mothers worldwide to breastfeed through mother-to-mother support, encouragement, information, and education, and to promote a better understanding of breastfeeding as an important element in the healthy development of the baby and mother.
© 2026 La Leche League Asia & Middle East, All Rights Reserved.
The images and written content contained in this website may not be used or reproduced in any way without express permission.
The images and written content contained in this website may not be used or reproduced in any way without express permission.