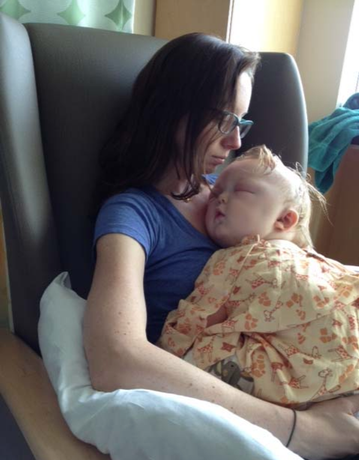
Just a few weeks earlier, Hunter had been diagnosed with a rare condition called craniosynostosis, and he was facing scary and invasive cranial surgery to correct it.
The first few months of Hunter’s life were far from easy. He was born in Hong Kong after a long but glorious drug-free labour. He latched almost immediately after he was placed on my chest, and it seemed that our breastfeeding relationship was off to a wonderful start. However, over the first few months of his life we battled reflux, colic, poor sleep, around-the-clock breastfeeding, clogged ducts and mastitis. I knew something was not right, and my own research helped me to identify a severe posterior tongue tie. Once that was corrected, our breastfeeding relationship quickly improved. Everything was great for several months. Hunter continued to have a large head (above the 99th percentile), but we never gave that much thought because he was also consistently above the 95th percentile for height and weight. Furthermore, none of the physicians who Hunter saw for well baby visits ever mentioned anything about his large and long (rather than round) head. Then, at Hunter’s 15-month checkup, the practitioner (almost just in passing) noted his prominent forehead and that there was a raised ridge running vertically down the middle of his skull. He commented that Hunter “might just have a big head” and suggested that we should simply keep an eye on it and follow up in a few years with a neurosurgeon. These observations were unsettling and we were not content to wait for a few years. Once home, I began searching the internet for clues. My Google searches consistently returned results for one condition over and over: sagittal craniosynostosis. Looking at images of children with the condition made my heart sink. I immediately made contact with a specialist educational and awareness organisation, and their representative quickly confirmed from photos that Hunter looked like “a typical sagittal synostosis child”. As the tears filled my eyes, I picked Hunter up and began to nurse him. It was my happy place, and in that moment of uncertainty it was the only thing that felt right. Oblivious to anything being wrong, Hunter happily nursed as I apologised profusely for not knowing sooner. I remember kissing away my salty tears that had fallen on his perfectly imperfect head and stroking the raised ridge that lay hidden under his beautiful and soft red hair. Craniosynostosis is a birth defect which occurs in one in 2,000 live births. In a nutshell, it means the premature fusion of one or more of the fibrous sutures of an infant’s skull. In Hunter’s case, the sagittal suture, which runs down the middle of the skull from the back fontanelle to the front, had fused too early, most likely in utero. This had caused his head to grow long and narrow and his forehead to protrude. It is a progressive deformity and as the brain continues to grow, the abnormal skull shape becomes more pronounced, leading to increased intracranial pressure, which can cause a myriad of neurological issues. In the coming days, we made arrangements for Hunter to be seen at Seattle Children’s Hospital, at its world-renowned craniofacial unit. Once there, a physical examination and CT scan confirmed a diagnosis of sagittal synostosis. Thankfully, all of Hunter’s testing showed that his brain was not currently under any increased pressure, so the decision to proceed with corrective surgery immediately was at our discretion. But the severity of the conditions that might result if we did not proceed (such as blindness, hearing loss, migraines and seizures, and developmental and learning delays) meant that we never had any doubts about going ahead with the surgery as soon as possible. We were given a surgery date three months in the future. My husband had to return to work in China until nearer the surgery date, while Hunter and I stayed with family in Seattle. Hunter would undergo a procedure called Cranial Vault Reconstruction (CVR). Basically, his skull plates would be removed, reshaped and then reaffixed using dissolvable plates and screws, resulting in a more normal head shape and ensuring his brain had plenty of room to continue to grow. Naturally, I had many concerns regarding this surgery. As a passionate breastfeeding mother, many of these concerns revolved around breastfeeding. When would I be able to breastfeed Hunter afterwards? Would the hospital allow it? Would he want to? How would I express milk during surgery and maintain supply afterwards if he didn’t want to breastfeed? In the month preceding Hunter’s surgery, I decided it was best to express some milk to have on hand after surgery, in case he wanted milk but couldn’t or wouldn’t latch to my breast. Since Hunter was usually only breastfeeding three times a day and I had never pumped before, expressing milk was no easy feat for me. I rented a hospital grade pump and began pumping after all Hunter’s nursing sessions. I found hand expression with breast compressions more useful than the pump, and managed to produce about half an ounce per session, which didn’t seem like much, but they all added up to 60 ounces over the course of a month, which I was very satisfied with. Looking back, it wasn’t really worth the effort because he only drank 8 ounces of it, although the routine and schedule of pumping gave me something to focus my worry and nervous energy on. I felt that I was preparing for surgery in some way, by doing something I knew I could, which was to make milk. Two days prior to the surgery, I had a battle with nurses regarding the latest time before surgery that Hunter would be allowed to breastfeed. I had done my own research and found the Academy of Breastfeeding Medicine’s “Recommendations for Pre-procedural Fasting for the Breastfed Infant”, which states that human milk can be safely ingested up to four hours before surgery. But a nurse phoned me to tell me that I had to stop breastmilk six hours prior to surgery, which meant they were classifying breastmilk in the same category as formula milk. She suggested that I offer pedialyte instead of breastmilk. I argued with her but she would not back down. I quickly emailed a nurse in the anaesthesiology clinic where Hunter and I had been for a pre-operative appointment a few weeks earlier, quoting the ABM’s four-hour guideline. The next day she responded that I was correct and told me Hunter could breastfeed up until four hours prior to surgery. This was a huge relief for me, to know we would have some sleepy early morning milk, which would make Hunter less grouchy about having to fast until 9am. I woke early on the morning of Hunter’s surgery. I quietly slipped into his room, picked up his warm body and latched him. He didn’t take much milk and was quickly back to dozy comfort nursing. I watched the clock and didn’t unlatch him until 4:59am, enjoying every last suckle but being able to confidently say he had stopped feeding by 5 am. Handing Hunter over to his surgeons was the most difficult thing I ever had to do. Once the surgery was in progress, my husband and I tried to keep busy. I quickly found a mothers’ room at the hospital to express milk, which was a useful distraction. In the afternoon, I had just begun setting up the pump for a second time when the pager we had been issued by the hospital went off: Hunter’s surgery had finished in under four hours, well ahead of the five to six hours we had been told to expect. The surgery had gone wonderfully and we were told we would be able to see him in the Intensive Care Unit shortly. He was still groggy but immediately responded to seeing us. Within minutes, Hunter was asking for water. He guzzled down 4 ounces of water and thankfully showed no signs of nausea. He drifted off for a nap and upon waking began to feverishly use sign language asking for milk. The nurse and my husband gingerly moved Hunter to my arms, being careful of all of his tubes and a drain he had coming out of his scalp. Once together, he immediately latched and we both felt at home again. I studied his beautiful new head while trying to get adjusted to how different he looked. Hunter didn’t take much milk before drifting back off to sleep while soothing himself at my breast.
About 30 hours after surgery, Hunter’s eyes swelled completely shut, which we had been told to expect. When he awoke from a nap to discover this, he immediately became disoriented and very upset. Breastfeeding helped him to feel safe when he couldn’t see. Thankfully, his eyes were back open about 36 hours later.
The hospital staff were incredibly supportive of us breastfeeding. They were thrilled at the number of wet diapers he was producing, and were happy that he was obtaining nutrition from me, since he had little interest in solid food. Hunter remained latched to my breast during the removal of IVs and the drain from his scalp, with barely a flinch. We spent three days in the hospital, Hunter being discharged after his eyes opened back up. He had a follow-up appointment with his surgeons just over three weeks after the surgery, and they were very pleased with how well he was healing. Days later, we made our way “home” to Guangzhou.
Close to the Heart Vol. 17, No. 1 (Early-Year 2016)
Please contact the editor for Close to the Heart at jennylllhk@gmail.com if you have a breastfeeding story you would like to share.
Comments are closed.
|
Close to the Heart ArticlesCategories
All
Close to the Heart is protected by copyright law. Reproduction and/or use in any form, by any means, graphically, electronically, or mechanically, is prohibited without permission.
|
Our Mission is to help mothers worldwide to breastfeed through mother-to-mother support, encouragement, information, and education, and to promote a better understanding of breastfeeding as an important element in the healthy development of the baby and mother.
© 2024 La Leche League Asia & Middle East, All Rights Reserved.
The images and written content contained in this website may not be used or reproduced in any way without express permission.
The images and written content contained in this website may not be used or reproduced in any way without express permission.